Variants responsible for 90 per cent of COVID-19 cases, ICU levels to remain high: latest modelling
Posted April 29, 2021 3:06 pm.
Last Updated April 29, 2021 4:33 pm.
This article is more than 5 years old.
The latest data reveals that over 90 per cent of COVID-19 cases in Ontario are caused by a variant of concern, with almost all being the B.1.1.7 variant first identified in the U.K.
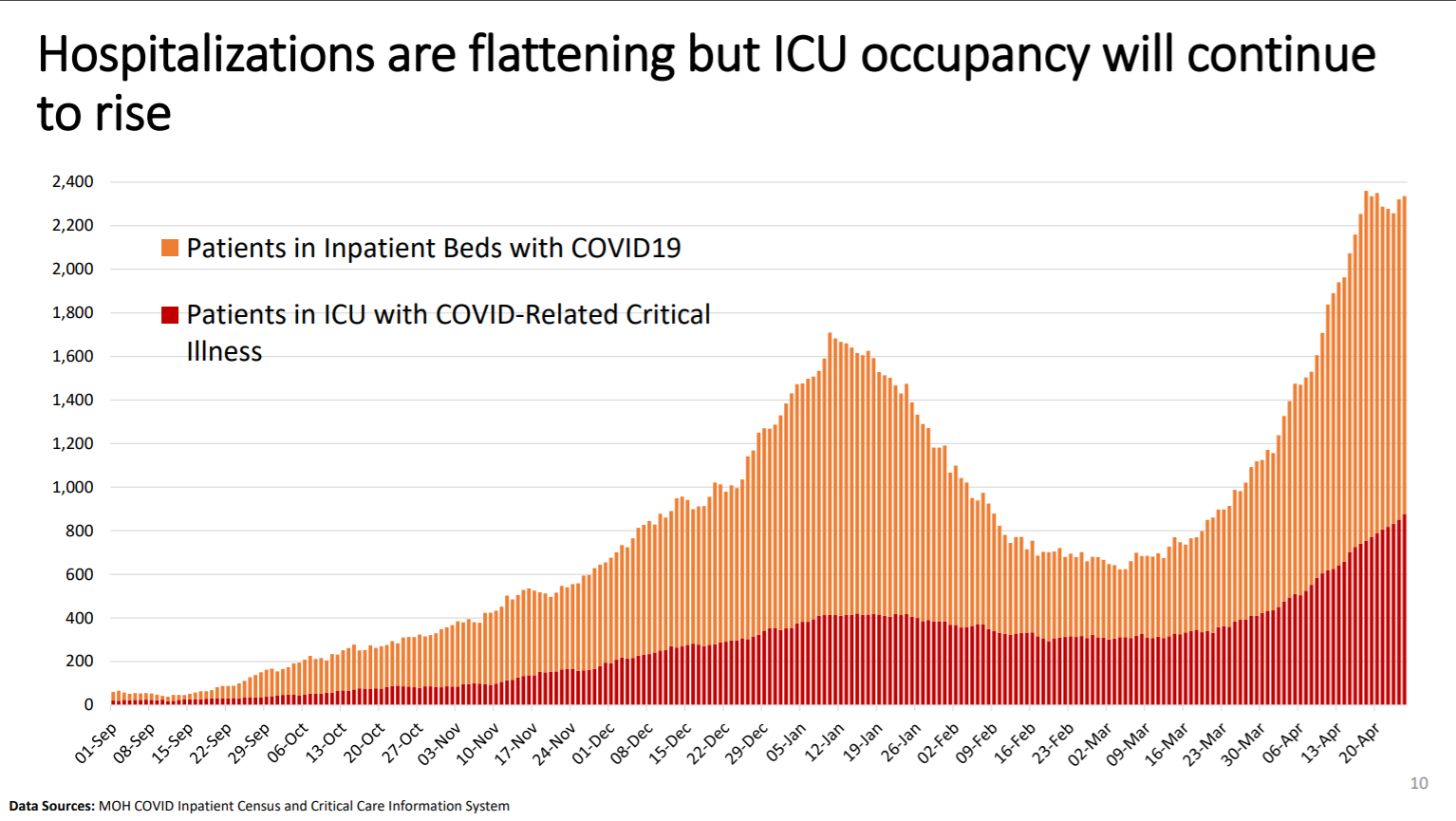
New modeling numbers show that while hospitalizations due to COVID-19 are levelling off, the number of patients in ICU with COVID-related critical illnesses is expected to continue rising.
ICU occupancy surpassed 800 around April 20 and under the best case scenario, the modelling suggests the numbers may come down to about 500 by the end of May. This is still not low enough to restart non-emergency surgeries for some time.
Dr. Adalstein Brown said that the number of patients in ICU was already still high as a result of the second wave when the third wave of the pandemic hit.
“It’s this occupancy of our Intensive Care Units which is such a significant threat currently to our health system,” he said.
“Our healthcare system is no longer functioning normally. We’re taking the most critically ill patients, we’re putting them in helicopters and in ambulances and moving them across the province because we’re searching for beds.”
The cumulative pandemic-related backlog of surgeries now stands at over 250,000 cases and officials say it poses an “enormous challenge.”
Further exposing the strain on the healthcare system is the fact that there has been a “dramatic rise” of patient transfers between hospitals. Dr. Brown says this is partly because some patients need to be sent to another hospital in order to get the care they need and partly due to intentionally moving patients to create more capacity in hospitals in the hardest hit communities.
While the third wave appears to be cresting and cases are flattening, growth continues in hotspots. Peel Region showed the highest per cent positivity rate, with a seven day average of 18.1 per cent on April 24. Toronto followed at 12.4 per cent and York Region at 10.7 per cent.
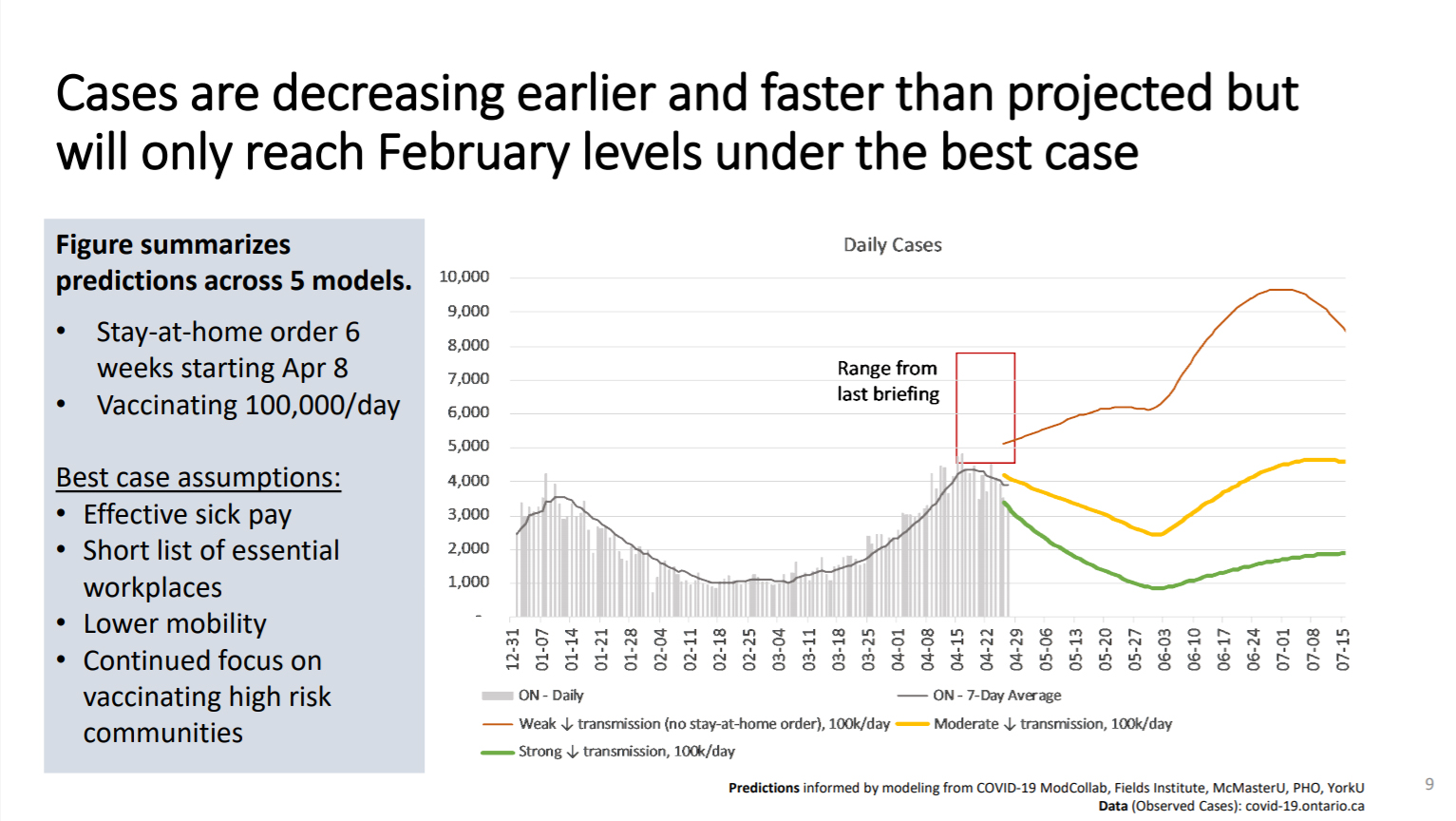
Cases are decreasing faster than expected, but even in the best case scenario, cases could begin to rise in June.
In the chart below, the yellow line represents where Ontario sits currently, with a six-week stay-at-home order in place and a vaccination rate of about 100,000 people per day. The red line represents where the province would have been had the stay-at-home order not been implemented.
“So there has been a substantial control of cases due to the stay-at-home order,” said Dr. Brown.
The case counts will only dip to the levels seen in February under the best case scenario, represented by the green line — which would require effective sick pay, a shorter list of essential workplaces, lower mobility and a continued focus on vaccinating high risk communities.
The reproduction rate of the virus – the possibility that someone may pass on COVID-19 to another person is at 0.9, which means the province is seeing a deceleration in cases. But Dr. Brown said it was important to remember that case counts remain very high.
“If we start to relax public health measures, after say six weeks which would have started on April 8, you can see there is a potential for an increase in cases again which can be quite dangerous given that our ICUs have not yet started to empty out in any way,” said Dr. Brown.
The data also shows that Ontarians are respecting the stay-at-home order, but workplace mobility is still too high. Brown said “limiting essential workplaces and keeping sick workers at home will help control cases.”
Vaccination numbers continue to grow and more than 4.5 million doses have now been administered in the province.
Around 36.6 per cent on Ontarians have received at least one dose of the vaccine, with the largest demographic still waiting for the first dose falling in the under 50 category.
Dr. Brown reiterated that prioritizing hotspot communities for vaccinations will help control the virus across the entire province.